The uterus |
|
Parts |
|
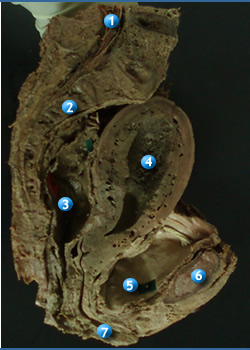
|
Body
Hover to show names
- Expanded superior 2/3rd
- Fundus- rounded superior part
- Cornu- part of the body where the uterine tubes insert
Isthmus
- A narrow cone
- Transition between the body and the cervix
- Most obvious in nulliparous women
Cervix
- Cylindrical inferior 1/3rd of the uterus
- Supravaginal part
- Infra vaginal part
- Internal/ external os
|
|
|
| Position |
|
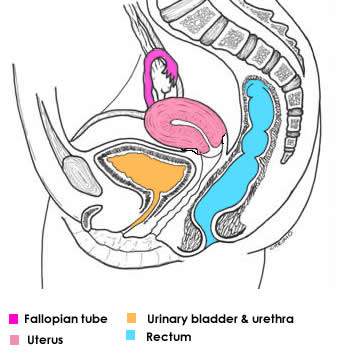 |
Anteflexed: Uterus is bent anteriorly over the bladder between the cervix and the body
Anteverted: The entire uterus is bend anteriorly with respect to the vagina
Sometime especially in older women, the uterus may be bent posterioly (retroversion)
Note: When the urinary bladder fills, the uterus is straightened into line with the vagina. |
|
Peritoneal relations |
|
|
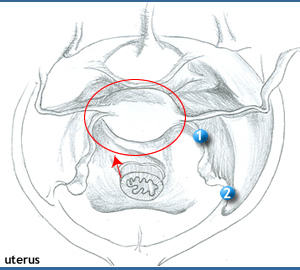 |
- Peritonioum covers , posterior, superior and anterior surfaces of the uterus, except vaginal part of cervix
- Peritoneum is reflected anteriorly onto the bladder and posteriorly onto the rectum
- A double layered peritoneal sheet - the broadligament- extend from the sides of the uterus to the lateral walls, and the floor of the pelvis.
|
|
| Relations |
|
Anteriorly
- Separated from urinary bladder by the vesico uterine pouch
- This pouch is normally empty when the uterus is in the normal position.
- When the uterus is retroverted the pouch contains a loop of intestine.
Posteriorly
- A layer of peritoneum and the peritoneal cavity separate the posterior part from sigmoid colon.
- The recto uterine pouch separates the uterus from the rectum.
Superiorly
- The coils of small intestine
Laterally:
- The broad ligaments and their contents
|
|
| Uterine support |
|
|
- The principal supports of the uterus are the pelvic floor and the pelvic viscera surrounding the uterus and its continuity with the vagina
- The broad ligaments hold the uterus in its relatively normal position.
- The body of the uterus is freely mobile. The cervix is not very mobile because it is held in position by several ligaments (Thickenings of the endopelvic fascia).
(+)
Transverse cervical (Cardinal) ligaments
(+)
Utero sacral ligaments (recto uterine),
(+) Pubocervical
|
|
Blood supply |
|
|
- Uterine arteries from the internal iliac
- Ovarian arteries from the aorta
- These two anastomose
- The uterine veins form a uterine venous plexus on each side of the cervix. Their tributaries drain into the internal iliac veins.
- This plexus is connected with the superior rectal veins forming a porto systemic anastomsis
|
|
Lymphatics |
|
|
- Aortic (lumbar) nodes.
- Superficial inguinal nodes.
- Body- para uterine lymph nodes thence to the external iliac nodes
- cervix – internal iliac and sacral lymph nodes.
|
|
Innervation |
|
|
- Autonomic from the inferior hypogastric plexus largely from the uterovaginal plexus in the broad ligament.
- Most of the efferent fibres ascend through the hypogastric plexus and the spinal cord via T10- L1 spinal nerves
|
|


