The Orbit
- Exopthalmos:
protrusion of the eyeball. Some causes include retrobulbar tumors such as lipomas, rhabdomyosarcomas, optic nerve schwannomas, orbital cellulitis and haematomas
- The thin orbital walls are easily fractured. This often causes the eyeball to sink causing enopthalmos
- The topographic relationship of the orbit with other cavities allows infections to spread easily between them
- Paralysis of the extraocular muscles may cause 'paralysis' of the eyeball or opthalmoplegia or deviation of the eyeball in one direction or another. This is called strabismus and often causes double vision- diplopia
- Impaired corneal reflex suggests damage to the sensory nerve (opthalmic) or motor (facial) or related brain stem centres
- Impaired pupillary responses suggest damage to parasympathetic pathways, oculomotor and sympathetic system as in Horner's syndrome
The Face
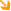 The face has a rich blood supply characterized by extensive anastomosis . Therefore lacerations bleed profusely and heal rapidly. Muscle contraction may gape wounds and hold vessels open, worsening the bleeding. The face has a rich blood supply characterized by extensive anastomosis . Therefore lacerations bleed profusely and heal rapidly. Muscle contraction may gape wounds and hold vessels open, worsening the bleeding.
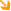 Veins of the upper face including the upper lips, nose, eyelids and forehead communicate with the cavernous venous sinus through: Veins of the upper face including the upper lips, nose, eyelids and forehead communicate with the cavernous venous sinus through:
- Ophthalmic veins
- Deep facial veins
Those of the forehead also communicate with the superior sagittal sinus through an emissary vein in foramen cecum.
These communications are potential routes for spread of infection from the face to the intracranial structure. For this reason, this part of the face is considered the danger area of the face.
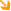 Injury to the facial nerve paralyses muscles of facial expression. Such paralysis is characterized by: Injury to the facial nerve paralyses muscles of facial expression. Such paralysis is characterized by:
- Deviation of the face to the normal side when the patient opens the mouth as in yawning or smiling
- Accumulation of food in the vestibule of the mouth – between the cheeks and teeth.
- Inability to close the eye causing corneal exposure and drying, hence vulnerability to ulceration
- Obliteration of nasolabial groove
- Loss of the corneal reflex on the affected side
|